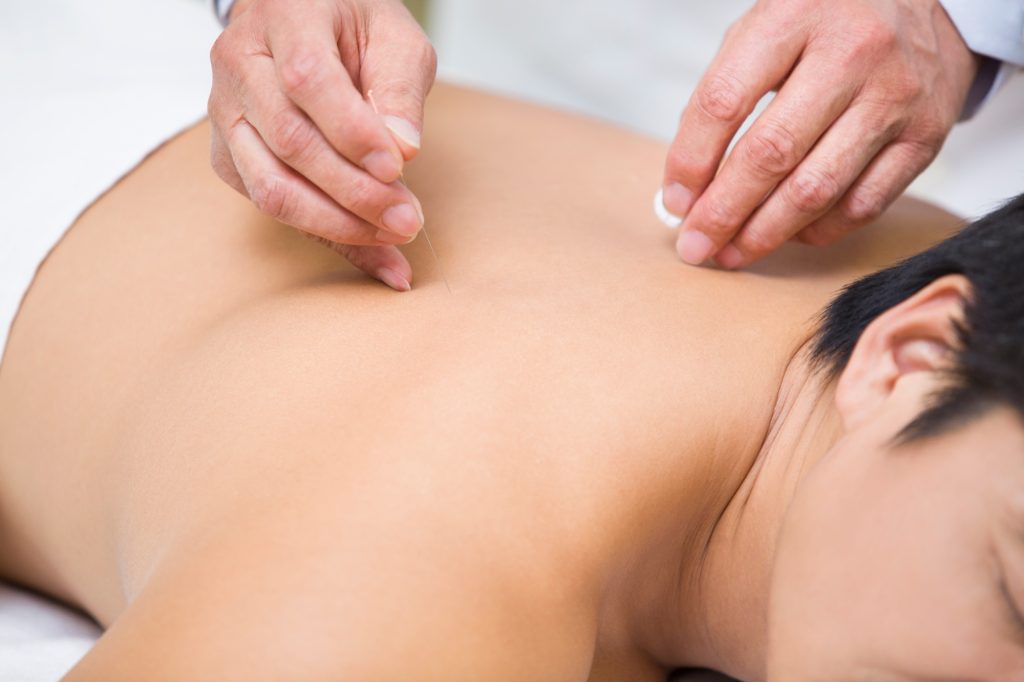
Acupuncture Therapy for Long Term Pain That Delivers Lasting, Evidence-Backed Relief
Acupuncture therapy for long term pain is a structured, clinically guided treatment that stimulates specific meridian points to regulate nervous system activity, improve blood circulation, and restore internal balance. Rather than masking symptoms, this therapy aims to address the root cause of persistent discomfort, whether musculoskeletal, neurological, or stress-related.
Long-term pain, also known as chronic pain, typically lasts more than 3 months and may involve conditions such as lower back pain, arthritis, migraines, neck tension, or nerve-related discomfort. Increasingly, patients across Australia and Singapore are turning to acupuncture therapy for long term pain as a natural, low-risk alternative or complement to pharmaceutical treatment.
Instead of relying solely on anti-inflammatory medication, acupuncture works by activating the body’s own regulatory systems, encouraging endorphin release, reducing inflammation, and improving nerve signalling. When performed by trained practitioners, outcomes are not only measurable but sustainable.
Understanding How Acupuncture Therapy for Long Term Pain Works
At its core, Acupuncture therapy for long term pain focuses on restoring the smooth flow of Qi (vital energy) through meridians connected to organ systems and musculoskeletal structures. In Traditional Chinese Medicine theory, chronic pain often arises when Qi and blood circulation become stagnant due to injury, repetitive strain, emotional stress, or internal imbalance. By stimulating specific acupoints, acupuncture reactivates these pathways, promoting natural healing and systemic regulation rather than temporary numbness.
From a biomedical perspective, growing clinical evidence explains why acupuncture therapy for long term pain produces measurable physiological effects. Research suggests acupuncture may:
- Stimulate endorphin and serotonin release
- Improve microcirculation
- Reduce inflammatory markers
- Modulate central pain processing pathways
- Calm overactive nerve signals
Endorphins act as the body’s natural painkillers, while serotonin contributes to mood stability and pain modulation. Enhanced microcirculation increases oxygen and nutrient delivery to affected tissues, accelerating repair. Studies also indicate that acupuncture influences cytokine levels, reducing inflammatory responses that perpetuate chronic discomfort.
Importantly, acupuncture therapy for long term pain does not only act at the site of pain. Functional MRI research shows that acupuncture can regulate activity within the brain’s pain matrix, including areas responsible for perception, emotional response, and sensory integration. This neuromodulatory effect explains why patients often report improvements not just in pain intensity, but also in sleep quality, stress tolerance, and overall function.
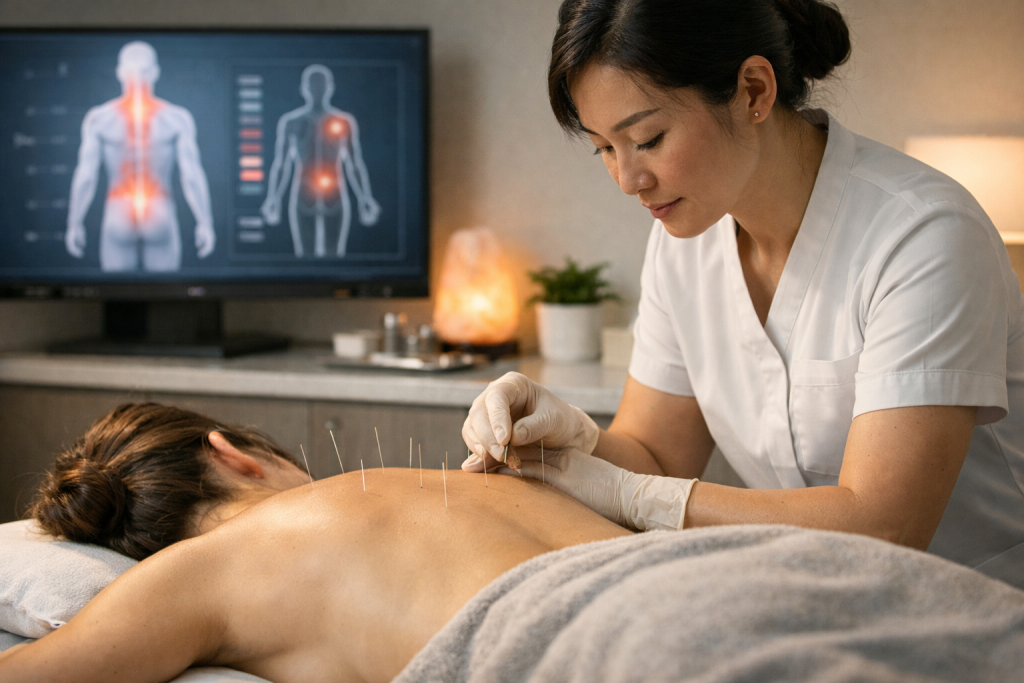
The World Health Organization World Health Organization recognises acupuncture as a therapeutic option for various pain-related conditions, reinforcing its global credibility and supporting its integration into multidisciplinary pain management programs worldwide.
The Biological Cycle of Chronic Pain and Neuromodulation
Chronic pain rarely develops overnight. It typically begins with repeated tissue stress caused by factors such as poor posture, overuse injuries, joint degeneration, or unresolved trauma. This prolonged strain triggers localized inflammation and nerve irritation. When inflammation persists, pain-signaling nerves become increasingly sensitive, sending stronger and more frequent signals to the brain.
Over time, the central nervous system may undergo a process known as sensitisation. In this state, the brain and spinal cord amplify pain perception, meaning discomfort can continue even after the initial tissue damage has improved. This explains why many individuals experience ongoing pain despite normal imaging results. The issue is no longer purely structural — it becomes neurological and functional.
Acupuncture therapy for long term pain works by intervening at multiple stages of this biological cycle. Locally, needle stimulation enhances blood circulation, reduces muscle tension, and promotes tissue repair. At the biochemical level, it regulates inflammatory mediators and stimulates the release of endogenous opioids such as endorphins. At the neurological level, acupuncture modulates pain-processing pathways in the brain, helping to recalibrate how pain signals are interpreted and transmitted.
Pro tip: Early intervention in chronic pain conditions often prevents long-term nerve sensitisation, making treatment more efficient and cost-effective.
Conditions Commonly Treated with Acupuncture Therapy for Long Term Pain
Many patients seek Acupuncture therapy for long term pain when conventional care provides limited improvement or when medication-based strategies lead to temporary relief without long-term resolution. Because acupuncture addresses both peripheral inflammation and central nervous system sensitisation, it is particularly beneficial for persistent, recurrent, and functionally limiting pain conditions.
Musculoskeletal Conditions
Acupuncture is frequently used to manage structural and movement-related pain disorders, including:
- Chronic lower back pain
- Neck and shoulder stiffness
- Osteoarthritis
- Sciatica
- Sports injuries
In musculoskeletal cases, chronic pain often results from muscle imbalance, joint degeneration, ligament strain, or nerve compression. Acupuncture helps reduce local inflammation, release myofascial tension, and improve blood flow to affected tissues. This enhances oxygen delivery and metabolic waste removal, supporting tissue repair. When applied systematically, Acupuncture therapy for long term pain also reduces compensatory movement patterns that may otherwise prolong recovery.
Neurological & Systemic Pain
Beyond structural pain, acupuncture is widely applied in neurological and centrally mediated pain conditions, including:
- Migraines
- Tension headaches
- Fibromyalgia
- Nerve-related discomfort
These conditions often involve dysregulation in pain-processing pathways rather than visible structural damage. Acupuncture modulates neurotransmitters such as serotonin and endorphins while stabilizing autonomic nervous system activity. This neuromodulatory effect helps decrease pain intensity, frequency, and hypersensitivity over time. For patients experiencing widespread or unexplained discomfort, acupuncture therapy for long term pain offers a regulatory approach rather than symptom masking.
A 2022 meta-analysis published in international pain journals found that acupuncture produced statistically significant improvement in chronic back and neck pain compared to standard care alone. Patients receiving structured acupuncture therapy for long term pain reported improved mobility, enhanced quality of life, and reduced reliance on analgesic medications, outcomes that highlight both functional and clinical relevance.
Pro tip: Combining acupuncture with posture correction and guided exercise accelerates recovery, improves musculoskeletal alignment, and stabilises long-term results.
Step-by-Step Treatment Framework
Before beginning the first stage of treatment, it is important to understand that Acupuncture therapy for long term pain follows a structured and progressive framework rather than a single-session intervention. Chronic pain develops through complex interactions between tissue stress, inflammation, and nervous system sensitisation, so effective management requires careful evaluation and strategic planning. Each step in the treatment process builds upon the previous one, ensuring that therapy is tailored to the patient’s specific pain mechanisms, constitutional patterns, and long-term recovery goals.
Comprehensive Health Consultation
Every session of Acupuncture therapy for long term pain begins with a structured and in-depth consultation. The practitioner explores not only the location and intensity of pain, but also its onset, progression, aggravating factors, prior treatments, and response to medication. Lifestyle elements such as occupational strain, posture habits, exercise routines, emotional stress, sleep patterns, and dietary influences are also evaluated.
Chronic pain rarely exists in isolation; it often reflects cumulative physiological stress or systemic imbalance. By gathering a complete health profile, the practitioner can identify underlying contributors, whether biomechanical overload, inflammatory tendencies, or nervous system dysregulation, ensuring that acupuncture therapy for long term pain addresses root mechanisms rather than surface symptoms alone.
Pain Pattern and Trigger Assessment
After the consultation, a focused physical assessment is conducted. The practitioner determines whether the pain is primarily inflammatory, neuropathic, muscular, myofascial, or stress-related. Movement testing evaluates joint mobility and muscular restriction, while palpation helps detect trigger points, tight fascia, or nerve sensitivity.
This stage is critical because chronic pain often involves overlapping mechanisms. For example, a patient with lower back pain may present both muscular tension and nerve sensitisation. Accurate pattern identification enhances the precision of Acupuncture therapy for long term pain and increases the likelihood of sustained improvement.
Pulse and Tongue Diagnosis (TCM Framework)
Within the Traditional Chinese Medicine framework, pulse and tongue examination provide additional diagnostic depth. Pulse qualities — such as wiry, slippery, thready, or weak. offer insight into circulation, energy flow, and systemic balance. Tongue characteristics, including color, coating, and moisture, help reveal internal heat, dampness, deficiency, or stagnation patterns.
When integrated with modern assessment, these traditional tools allow practitioners to differentiate whether pain is rooted in Qi stagnation, blood deficiency, cold obstruction, or damp accumulation. This pattern-based analysis strengthens the effectiveness of acupuncture therapy for long term pain by aligning treatment with the patient’s constitutional profile.
Personalised Point Selection
Acupuncture points are selected strategically based on both local pain regions and systemic regulatory needs. Local points target muscle tension, inflammation, and restricted mobility, while distal points along meridians influence broader neurological and circulatory pathways.
Research suggests that stimulating specific acupoints activates peripheral nerves that communicate with the spinal cord and brain, promoting endogenous opioid release and neuromodulation. By combining anatomical understanding with meridian theory, Acupuncture therapy for long term pain delivers a multi-layered therapeutic response rather than isolated tissue intervention.
Needle Insertion (Typically 15–30 Minutes)
Fine, sterile, single-use needles are inserted at controlled depths appropriate to the anatomical region. Most patients experience mild sensations such as warmth, tingling, or a dull ache, often described as the “deqi” response in TCM. This sensation indicates activation of sensory nerve fibers and local microcirculation.
During the retention period, typically lasting 15–30 minutes, physiological changes occur at multiple levels. Blood flow improves, inflammatory mediators decrease, and central pain-processing pathways begin to recalibrate. In structured acupuncture therapy for long term pain, consistent stimulation over several sessions supports cumulative neuromodulatory adaptation.
Post-Treatment Evaluation
At the conclusion of the session, the practitioner reassesses pain intensity, joint mobility, muscle tightness, and overall response. Immediate improvements may include reduced stiffness or enhanced range of motion, although deeper neurological recalibration develops progressively.
Future sessions are adjusted based on response patterns, ensuring that treatment remains dynamic and responsive. This ongoing evaluation phase distinguishes acupuncture therapy for long term pain from static treatment models, reinforcing a precision-based approach designed for sustainable recovery rather than temporary relief.
Session Experience
Most patients describe:
- Mild tingling or warmth
- Deep muscle relaxation
- Reduced tightness after the session
- Gradual cumulative improvement over multiple treatments
Pain reduction often occurs progressively rather than instantly, particularly in chronic cases. Consistent sessions help retrain pain-processing pathways and restore systemic balance.
If you’d like to explore how acupuncture supports overall regulation beyond pain relief, you may read more about acupuncture for body balance, which explains its broader physiological effects.
Pro tip: Consistency matters more than intensity, weekly sessions during the initial phase often produce more stable neuromodulatory changes and prevent relapse in chronic pain conditions.
Comparing Acupuncture Therapy for Long Term Pain with Conventional Management
When evaluating chronic pain management options, patients often weigh the differences between non-pharmacological therapies and medication-based approaches. While both aim to reduce discomfort and improve function, their mechanisms, sustainability, and long-term implications can differ significantly.
| Feature | Acupuncture Therapy for Long Term Pain | Medication-Based Care |
|---|---|---|
| Approach | Root cause modulation | Symptom suppression |
| Side Effects | Minimal when professional | Possible gastrointestinal or systemic |
| Long-Term Sustainability | High | Variable |
| Nervous System Regulation | Yes | Limited |
| Dependency Risk | None | Possible with certain drugs |
While medication may provide immediate relief, acupuncture therapy for long term pain often builds progressive improvement without pharmacological dependency.
Clinical Outcomes and Observed Benefits
In structured clinical settings:
- 70–80% of chronic back pain patients report measurable relief within 5–8 sessions
- Migraine frequency may reduce by up to 50% after consistent treatment
- Sleep quality often improves within 3 sessions
- Reduced reliance on anti-inflammatory medication observed in long-term follow-up
Patients frequently report improved mood and energy levels, indicating systemic regulation rather than isolated symptom control.
Pro tip: Adequate hydration after sessions enhances circulation and supports detoxification pathways.
Exploring Professional Acupuncture Services
Structured acupuncture therapy for long term pain should be performed by licensed practitioners trained in both Traditional Chinese Medicine principles and modern clinical assessment.
If you are reviewing available services and treatment options, you can explore professional acupuncture offerings through the clinic’s overview of TCM acupuncture services, which outlines diagnostic frameworks and therapy protocols.
Modern clinics may integrate:
- Electro-acupuncture
- Infrared heat therapy
- Cupping therapy
- Herbal support
This integrated model strengthens the effectiveness of acupuncture therapy for long term pain.
Conclusion: Taking Control of Chronic Pain with Structured Acupuncture Care
Living with persistent discomfort can be exhausting, physically and emotionally. The good news is that acupuncture therapy for long term pain offers a clinically grounded, low-risk pathway toward sustainable relief. By targeting nervous system regulation, circulation, and inflammation simultaneously, it provides more than temporary comfort, it supports genuine functional recovery.
If you are considering professional evaluation and personalised treatment, you may explore further information about practitioner credentials and integrated care models through the official site of GNG TCM. Understanding your options is the first step toward structured, evidence-informed pain management.
Chronic pain does not need to define your daily routine. With proper diagnosis, consistent care, and a holistic strategy, meaningful improvement is achievable.
Pro tip: The earlier chronic pain is addressed, the less likely it is to become neurologically entrenched, early action often leads to faster recovery.
FAQs Section
How many sessions are needed for chronic pain?
For chronic pain conditions such as arthritis, lower back pain, or long-standing neck tension, most patients begin with 6–10 sessions over several weeks. Unlike painkillers that provide temporary relief, acupuncture therapy for long term pain works by gradually regulating circulation, reducing inflammation, and stimulating the body’s natural healing response. Improvement is typically cumulative, meaning each session builds upon the previous one. Severe or long-standing conditions may require additional maintenance sessions to stabilise results and prevent flare-ups.
Does acupuncture therapy for long term pain hurt?
Acupuncture needles are extremely thin, much finer than injection needles, so discomfort is usually minimal. Patients commonly describe sensations such as tingling, warmth, mild pressure, or heaviness rather than sharp pain. These sensations are often associated with the therapeutic response known as “De Qi,” which indicates that the point is being effectively stimulated. Any slight discomfort typically subsides quickly, and many people report feeling deeply relaxed during and after treatment.
Is acupuncture safe for elderly patients?
Yes, acupuncture is generally safe for elderly patients when performed by licensed and trained practitioners. It is frequently used to manage age-related conditions such as osteoarthritis, joint stiffness, sciatica, and mobility-related discomfort. Treatment plans are usually adjusted to suit an older patient’s overall health condition, medication use, and sensitivity levels. Gentle techniques and careful point selection help ensure both safety and comfort throughout the therapy process.
Can acupuncture replace pain medication?
In some cases, patients may gradually reduce their reliance on pain medication after experiencing consistent improvement with acupuncture. However, acupuncture should not abruptly replace prescribed medication without medical supervision. A coordinated approach involving both the acupuncturist and primary healthcare provider ensures safe integration, particularly for patients managing chronic conditions that require long-term pharmaceutical support. The goal is often to complement conventional care and potentially lower medication dependency where appropriate.
Are results permanent?
The longevity of results depends on several factors, including posture, physical activity, stress levels, occupational strain, and overall lifestyle habits. While many patients experience long-lasting relief after completing a treatment course, chronic pain conditions may require periodic maintenance sessions to sustain improvement. Acupuncture therapy for long term pain focuses on restoring balance and function, and maintaining those results often involves supportive exercises, ergonomic adjustments, and stress management practices.